High arch foot is a congenital condition.
Pes cavus, often called high arch, is a kind of human foot in which the sole of the foot is hollow when bearing weight. Neurological problems, such as tethered cord syndrome, syringomyelia, and genetic neurological disorders, cause a small number of congenital diseases, the majority of which affect children under the age of three.
What is a high arch, exactly?
When carrying weight or walking, a high arch is defined as a significant elevation in the longitudinal arch on the inside and outside of the foot that does not flatten out. The flexibility of the feet decreases when walking or loading, and the pressure on the front and rear of the feet increases. Approximately 15% of the general population and 25% of athletes have high arches.
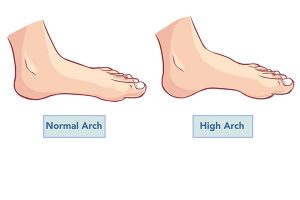
Vector – vector illustration of a high arch and normal feet
The root of the problem
The cause of a high arch foot has yet to be discovered. There is a family history of disease in certain unexplained high arches, and it is suspected that genetic factors are involved in the pathophysiology, but there is no genetic evidence.
Presentation at the clinic
The patient exhibits symptoms and indicators that range in severity according on the degree of deformity:
1. High arch, horseshoe, and claw-shaped toes were the most common abnormalities. The longitudinal arch of the foot is taller, the length of the foot is shorter, and the metatarsophalangeal and interphalangeal joints are in dorsiflexion and plantar flexion, respectively. Achilles tendon contracture, plantar aponeurosis contracture, anterior tibial muscle weakening The skin of the metatarsal head on the sole of the foot can develop calluses and even necrosis.
2. Most patients are unable to walk for lengthy periods of time, experience foot tiredness, and experience soreness.
3. Feet that are inelastic and have limited dorsiflexion.
4. The amount of time the soles of the feet are in contact with the ground is reduced. The deformity light person, on the other hand, stands when the weight-bearing deformity diminishes or even vanishes, and the footprint returns to its original shape.
What distinguishes high arches from other types of arches?
1. Standing or walking with the heel striking the calcaneus varus, walking in a figure eight pattern, increasing the frequency of walking, and not being able to stop feeling.
2. The arch of the foot is obviously raised, and the surface of the foot is obviously higher than the average person; when buying shoes, there is often a feeling of being unable to take them off; the pronation of the foot is insufficient, resulting in obvious wear marks on the outside of the shoes and the little toe.
3. The sole and toe muscles are particularly stiff; the old callus below the big toe or the foot 5 toe is more prominent, and the toe or cocked toward the dorsal side has calluses;
4. In addition to the above simple method, the high arch foot can be tested on professional equipment to obtain a more detailed plantar pressure map, center of gravity transfer line, or foot 2D 3D scan image; in the X Ray Display, the medial longitudinal arch was clearly increased, the first metatarsal head was clearly stressed, and the toe was turned up.
Make a check
The foot should be photographed when loaded during the x-ray examination. The distal and proximal first cuneiform bones’ joint surfaces are parallel in the normal foot, however those with a high arch foot have plantar flexion deformity, which primarily occurs in the first cuneiform joint. M ′ eary angle was used to determine the angle between the talus axis and the axis of the first metatarsal. The arch of the foot is lifted if the angle can be measured.
Hibbs calculated the angle between the calcaneus axis and the first metatarsal axis. The usual temperature range was 150° to 175°. The angle is lowered with high arches. Furthermore, if the heel angle is less than 20 degrees, it suggests that the back foot is varus deformed.
Differential diagnosis and diagnosis
An irregular stride, elevation of the longitudinal arch of the foot with claw-shaped toe deformities, and rise of M ′ eary angle and decrease of Hibbs angle might all be signs of a high arch foot. Electromyography, head or spinal CT, or MRI should be used to look for primary disease or probable etiologic factors in deformities caused by neuromuscular illnesses with high arches. Understanding the etiology of sickness is critical in determining the prognosis.
Medications
1. The treatment’s purpose is to alleviate discomfort, enhance foot function, and repair and prevent abnormalities from worsening.
2. Slight deformity, good foot flexibility, standing weight-bearing high bow deformity can be reduced or eliminated, low-heeled orthopedic shoes can be used, and callus plus metatarsus pad is present.
3. Surgery is required for moderate and severe deformities:
(1) The metatarsal aponeurosis is appropriate for spastic high arch feet and may be continued beyond one year. When the dorsum of the forefoot is stretched, the anterior part of the medial malleolus should be cut off at the most tensing region of the plantar fascia, and the plaster cast should be placed for 4 to 6 weeks following the operation.
(2) Tendon transfer of the extensor hallucis longus is appropriate for paralytic high arch feet. To prevent forefoot prolapse, the extensor hallucis longus muscle was relocated back to the first metatarsal head to become the dynamic tendon. The extensor digitorum tendon can be pushed back at the same time as the metatarsal contracture soft tissue is relaxed, if necessary. Three months of postoperative plaster fixing were required.
(3) For large children or adults with substantial deformities, midtarsal osteotomy, tarsal osteotomy correction, and triple arthrodesis are appropriate procedures. The V-shaped tarsal osteotomy of the dorsalis pedis offers several advantages, including the fact that it does not injure the tarsal epiphysis, making it appropriate for children over the age of six. The utility model does not shorten the foot and can address the forefoot deformities of adduction and pronation. The following are the major points of the operation:
1) Make a transverse or longitudinal incision on the dorsum of the foot, exposing the tarsus bone from the periosteum.
2) At the peak of the arch of the foot, which was placed in the center of the scaphoid, a v-shaped osteotomy line was established, and the medial ramus was slanted from the scaphoid to the medial cortex of the first cuneiform.
3) The anterior foot was dragged toward the distal end and lifted following osteotomy, while the distal end was forced down. If the pronation, or adduction deformity, is present, the forefoot external rotation, or abduction, may be used to remedy the problem. A Kirschner wire is then passed from the medial side of the first metatarsal to the lateral part of the calcaneus via the osteotomy line. The limb was plastered for six weeks after the operation. The Kirschner wire was removed once the plaster was removed, and the osteotomy healing was monitored with an X-ray. Start walking with a hefty weight once you’ve been healed.
The prognosis
Short-term treatment is preferable, although the danger of postoperative recurrence must be considered.
What are the things that people with high arched feet should be aware of?
1. Choose a pair of shoes that are comfortable for you. Because the inner side of the foot is not strong enough to take additional force from the ground, people with high arched feet should wear shoes that are stable and have good shock absorption. They should avoid wearing flats or loafers.
2. Change the way you walk. Enhance the pronation of the foot as much as possible in the center of the standing position, increase the flexibility of the middle foot, in short, can be their own suitable foot activities every day, walking speed is not too fast.
I’m going to murder you. Reduce the tension in the tibialis anterior, tibialis posterior, peroneus longus, plantar fascia, and calf triceps muscles. Simply put, you can massage your legs and feet on a daily basis from front to back, from inside to outside.
4. Place the orthotic insole in place. Cushioning, supporting, and rolling are the three main functions of the foot. The right orthotic insole can improve arch support, promote pronation in the middle foot, and transfer pressure from the heel to the first or fifth metatarsal bones, preventing additional knee, hip, and lower limb compensation.
Hot blogs:
The Easiest Custom Insoles: Heat Moldable Insoles
Custom insoles, also known as orthotic insoles, are designed to provide personalized support and comfort for individuals with various foot conditions. In [...]
Children’s Insole Size Conversion Chart
The standard sizes for shoe insoles may vary from country to country, making it a headache to choose the right insole for [...]
Do custom orthotics need to be made by a doctor personally?
Custom orthotics do not necessarily need to be made by a doctor personally. While doctors, specifically podiatrists or orthopedic specialists, are often [...]
Do NBA players use custom insoles?
Custom insoles are not only helpful for people with foot health issues, but they also play a significant role in targeting the [...]
