diabetic foot ulcers
Diabetes patients are called diabetes foot due to foot infections, ulcers, and/or deep tissues caused by distal vascular lesions and nerve abnormalities in the lower limbs. The incidence of diabetic feet in diabetic patients over 50 years of age in my country is as high as 8.1%. Foot ulcer is the most common manifestation of diabetic foot. About 25%of patients with diabetes will have foot ulcers. More than 85%of the lower limb amputation is caused by foot ulcers.
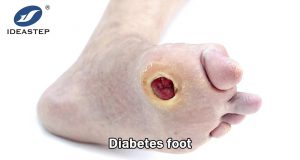
What are the causes of diabetic foot ulcers? First, vascular lesions. It mainly refers to the main cause of amputation of the foot of the lower limb arterial occlusion (PAD), which is the main cause of amputation, and often causes ulcers after mild trauma. Second, neuropathy. Some patients may have a burning sensation, acupuncture, numbness, and night pain; some patients feel lack of painless symptoms, and these painless patients often cannot feel the damage of the content and more prone to ulcers. The autonomous neuropathy of the lower limbs leads to reduced sweating, and the skin is dry and cracking; those with short -circuited veins can increase local blood flow and increase the skin temperature. Third, diabetic foot bone deformities can cause local stress concentration and cause foot ulcers.
The treatment of diabetic foot ulcers includes decompression, infection, and increased blood supply. The decompression can be used to use the full -contact plaster branches (TCC), which can change the tissue of the ulcer tissue, reduce the inflammatory response, and promote wound healing. Anti -infection therapy includes local debridement drainage and targeted antibiotics. Increasing blood supply to the treatment includes early drug treatment, high -pressure oxygen, and the rapidly developing tibial horizontal bone handling surgery in China in recent years.
Prevention of diabetic foot ulcers. The most important part of reducing the amputation rate of diabetes is to prevent and treat early treatment of diabetic foot ulcers. The first is the screening of diabetic foot, including medical history inquiries, appearance and imaging performance, vascular and neurological examination. Common examinations include foot arterials, custody, leather temperature testing, ankle -like measuring, 10g nylon wire examination and other methods. For patients with diabetes foot, be careful not to walk barefoot to avoid damage to the skin; do not soak your feet with hot water; wear loose cotton socks; use sugar -footed insoles or shoes; cutting toenails too deeply to prevent parameteritis; quit smoking; control blood glucose; control blood glucose; control blood glucose; blood pressure.
In summary, sugar -sufficient prevention and control requires multi -disciplinary cooperation, professional control and prevention. Medical professionals participating in diagnosis and treatment at different stages of foot ulcer may be different, and they need to work together to cooperate with internal and surgical medical staff and patients and family members.


For more information, please visit
https://www.aideastep.com/product/medical-diabetic-insoles-shoe-inserts-non-smell-foam/
